Cestodes
Human infections caused by cestodes (tapeworms) may occur within the lumen of the bowel, where adult cestodes attach to the host intestine (Table 1). Alternatively, human infection may result from dissemination of cestodes from the bowel to extraintestinal sites, often by larval forms of the parasite. The life cycle of cestodes is determined by definitive hosts, in whom the mature adult worm lives, and intermediate hosts, which harbour the larval forms of the parasite. Understanding which host is involved, and whether disease is intestinal or extraintestinal, helps clinicians anticipate potential complications and select appropriate diagnostic tests.
Humans are definitive hosts for six cestodes: Diphyllobothrium latum, Taenia solium, Taenia saginata, Hymenolepis diminuta, Hymenolepis nana, and Dipylidium caninum. In addition, humans may be intermediate hosts for Echinococcus granulosus and Echinococcus multilocularis. All forms of disease associated with cestode infections are treatable; therefore, it is important to take a careful history and perform a physical examination to identify patients at risk. Asking about travel, dietary exposures, contact with animals, and sanitation can be particularly helpful in raising suspicion of tapeworm infection.
Cestodes attach to the intestinal mucosa by means of a specialised organ called the scolex, which has a distinctive morphology for each cestode species. Attached to the scolex are one to several hundred segments called proglottids. Each proglottid contains both male and female reproductive organs and may be classified as immature, mature, or gravid, based on the maturation of the sex organs. A gravid proglottid contains a fully developed uterus that is full of eggs. The uterine structure of a gravid proglottid helps differentiate cestode species. These anatomical differences are important because they allow laboratory personnel to distinguish among species when examining stool specimens.
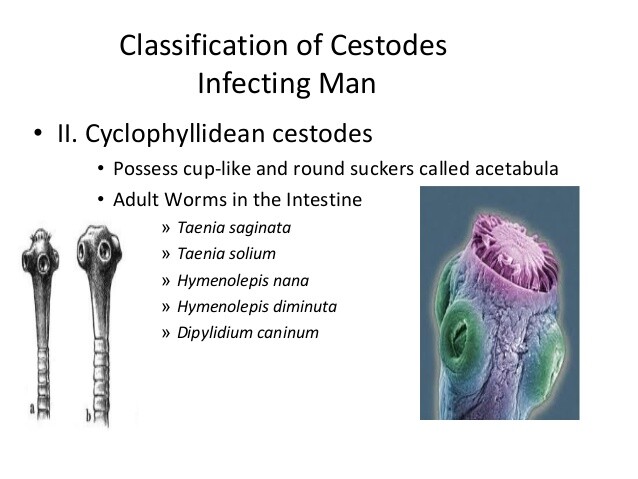
This classification figure summarises the major human cestode species and illustrates how intestinal and extraintestinal infections are related across different hosts and life-cycle stages.
Hymenolepis nana infection
Essentials of Diagnosis
- Adult worms and proglottids are rare.
- Spheroidal, thin-walled eggs (30-47 µm).
- Eggs contain two polar elements from which 4-8 filaments project (diagnostic).
- Scolex has hooklets and four suckers.
General Considerations
Hymenolepis nana (H nana) is distributed worldwide and is called the dwarf tapeworm because of its small size, measuring about 0.8-1.6 inches (2-4 cm). Endemic areas include Asia, Africa, South and Central America, and southern and eastern Europe. Infection with H nana is acquired by ingesting eggs, commonly from human stool. The eggs hatch within the stomach or small intestine, and the resultant larvae attach to the bowel wall, where adult worms develop over several weeks. Eggs are released directly from the gravid proglottids while these proglottids are still attached to the adult worm; therefore, proglottids are rarely seen on stool examination. Various arthropods, such as fleas, can serve as alternate intermediate hosts for H nana. Eggs produced within infected humans can lead to internal autoinfection, and poor faecal-oral hygiene can allow infection to pass from one person to another. Crowding, limited access to sanitation, and close contact among household members may all facilitate transmission.
Clinical Findings
Signs and Symptoms
Infection with H nana is most often asymptomatic, although some patients may report headache, dizziness, anorexia, or abdominal pain. Whether these symptoms are related to the infection is uncertain. Children may have headache or sleep and behavioural disturbances, which resolve after successful treatment of the infection. When symptoms are present, they are usually mild and non-specific, so a high index of suspicion is needed to consider tapeworm infection.
Laboratory Findings
As in other cestode infections, blood examination in patients with H nana infection is typically normal, although mild leukocytosis with eosinophilia may be present. Microscopic stool examination frequently reveals eggs, but finding proglottids is uncommon in H nana infection. Repeated stool examinations or concentration techniques may improve the likelihood of detecting eggs when clinical suspicion remains high.
Differential Diagnosis
Because infection with H nana is usually asymptomatic, it is most often discovered incidentally on a stool examination performed for another reason. In patients with non-specific gastrointestinal complaints, peptic ulcer disease and malignancy need to be ruled out. Similarly, in children with behavioural symptoms, a range of neurological disorders with organic and psychological causes need to be considered. Other intestinal parasites and functional gastrointestinal disorders may also be included in the differential diagnosis, depending on the clinical context.
Complications
Seizures have been reported in association with H nana infections through a mechanism that remains unclear. Although uncommon, these neurological manifestations underscore the importance of evaluating and treating confirmed infections, and monitoring patients with new or unexplained neurological symptoms.
Treatment
Cysts of H nana are more resistant to therapy than adult worms. Therefore, higher doses or longer courses of therapy are required to eradicate cysts than in other cestode infections. Therapy for H nana infection consists of a single dose of either praziquantel or niclosamide (see Table 2). Follow-up stool examinations should be performed at 2 weeks and 3 months after therapy. Treatment decisions, including drug choice and dosing, should be made in consultation with a healthcare provider, taking into account age, comorbidities, and potential drug interactions.
Prognosis
Because H nana infection is usually asymptomatic and responds to therapy, the prognosis is excellent. Relapse or reinfection is more likely in settings with ongoing exposure, so attention to household contacts and environmental conditions is helpful.
Prevention & Control
Infection with H nana can be prevented through good faecal-oral hygiene and adherence to sanitation principles (eg appropriate disposal of human sewage) (Table 3). Incidental ingestion of arthropod hosts may also cause infection, although this route is uncommon. Handwashing with soap and water, safe food handling, and control of household pests all contribute to reducing the risk of infection and reinfection.
Hymenolepis diminuta
Essentials of Diagnosis
- Proglottids are rare in stool, but adult worms may be present.
- Ovoid, thick-walled eggs (70-85 µm by 60-80 µm).
- Eggs contain no polar elements.
- Scolex has no hooklets and four suckers.
General Considerations
Hymenolepis diminuta is also distributed worldwide, but the incidence of infection is much lower than for H nana. Infection with H diminuta is acquired by ingesting eggs produced from an obligatory arthropod intermediate host. The eggs hatch within the stomach or small intestine, and adult worms develop over several weeks. The eggs are similar in size to those of H nana but can be distinguished by their ovoid shape and lack of polar filaments. In contrast to H nana, the life cycle of H diminuta requires an intermediate arthropod host, and adult worms may be passed in human stool. Human infection is usually sporadic and is often associated with inadvertent ingestion of infected insects in food or the environment.

This illustration highlights the general structure of cestodes, including the scolex and chains of proglottids, which are shared features across many tapeworm species.
Clinical Findings
Signs and Symptoms
Infection with H diminuta is not associated with clinical symptoms. Most cases are discovered incidentally, and patients usually remain well even when the infection is identified.
Laboratory Findings
Microscopic stool examination frequently reveals eggs and adult worms. Blood examination may demonstrate mild leukocytosis with eosinophilia. As with other helminth infections, the degree of eosinophilia does not always correlate with symptom severity.
Differential Diagnosis
Detection of H diminuta in humans is commonly an incidental, asymptomatic finding. Other causes of eosinophilia, intestinal discomfort, or abnormal stool tests should be evaluated when the clinical picture is not fully explained by this tapeworm infection.
Complications
No complications have been reported. Nevertheless, consultation with a healthcare professional is appropriate to confirm the diagnosis and determine whether treatment is indicated.
Treatment
Therapy for H diminuta infection consists of niclosamide as a one-time dose. Specific dosing regimens should be selected and supervised by a healthcare provider, particularly for children and individuals with underlying medical conditions.
Prognosis
H diminuta responds promptly to therapy, so the prognosis is excellent.
Prevention & Control
Infection with H diminuta can be reduced by decreasing exposure to arthropod vectors, such as through rat control measures (Table 3). Measures to protect stored grains and food from rodent and insect contamination also help reduce the risk of infection.
| Syndrome | More common manifestations | Less common manifestations |
|---|---|---|
| Diphyllobothrium latum infection | Bloating, abdominal pain, diarrhoea | Intestinal obstruction, vitamin B12 deficiency |
| Taenia solium infection | Asymptomatic | Indigestion, nausea |
| Cysticercosis (extraintestinal T solium infection) | Headache, seizures, neurological deficits | Myositis, liver or heart failure |
| Taenia saginata infection | Asymptomatic | Abdominal cramps, malaise |
| Hymenolepis nana infection | Abdominal pain | Dizziness, anorexia; in children, behavioural disturbance |
| Hymenolepis diminuta infection | Asymptomatic | |
| Dipylidium caninum infection | Asymptomatic | Indigestion, anorexia, anal pruritus |
| Echinococcal infection | Abdominal pain, mass | Seizures, headache, neurological deficits, bone pain |
| Syndrome | Adult treatment | Paediatric treatment |
|---|---|---|
| Diphyllobothrium latum infection |
|
|
| Taenia solium infection |
|
|
| Cysticercosis (extraintestinal T solium infection) |
|
|
| Taenia saginata infection |
|
|
| Hymenolepis nana infection |
|
|
| Hymenolepis diminuta infection |
|
|
| Dipylidium caninum infection |
|
|
| Echinococcal infection |
|
|
| Syndrome | Prevention and control measures |
|---|---|
| Diphyllobothrium latum infection | Adequate cooking of fish or freezing fish for 48 hours |
| Taenia solium infection | Adequate cooking of pork or pork products |
| Cysticercosis (extraintestinal T solium infection) | As for T solium |
| Taenia saginata infection | Adequate cooking of beef and beef products; inspection of beef and destruction of infected carcasses |
| Hymenolepis nana infection | Adherence to good faecal-oral hygiene |
| Hymenolepis diminuta infection | Arthropod control measures (such as rat control) |
| Dipylidium caninum infection | Screening of dogs and cats; treatment of infected animals |
| Echinococcal infection |
|

















