Condylomata acuminata
Description of Medical Condition
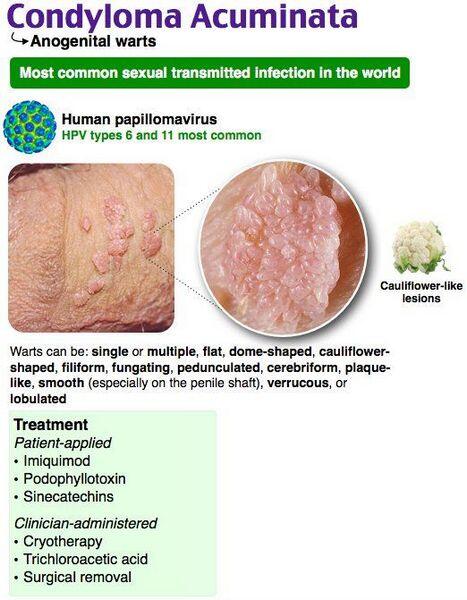
Condyloma acuminata are soft, skin-coloured, fleshy warts caused by HPV (human papillomavirus). There are now > 100 known types of HPV, and types 6, 11, 16, 18, 31, 33, and 35 have been associated with condyloma acuminata. The disease is highly contagious and can appear singly or in groups, and may be small or large. Lesions can appear in the vagina, on the cervix, around the external genitalia and rectum, in the urethra and anus, and also as conjunctival, nasal, oral, and laryngeal warts, and occasionally in the throat. The incubation period may be from 1-6 months.
System(s) affected: Skin/Exocrine, Reproductive
Genetics: N/A
Incidence/Prevalence in USA:
- Most common viral sexually transmitted disease in the U.S.
- ≥ 1% of sexually active population in U.S. has genital warts
- 26% transmission after single encounter
- Minimum of 10-20% of sexually active women may be infected with HPV. Studies in men suggest a similar prevalence.
- 750,000 new cases per year; rates are increasing
- Peak prevalence is in ages 17-33
- Pregnancy and immunosuppression favour recurrence and increasing growth of lesions
Predominant age: 15-30 years of age
Predominant sex: Male = Female
Medical Symptoms and Signs of Disease
- Tumours, soft, sessile
- Surface smooth to very rough
- Multiple fingerlike projections
- Perianal condylomata acuminatum usually rough and cauliflower-like
- Penile lesions are often smooth and papular
- Penile lesions often occur in groups of three or four
- Male sites - frenulum, corona, glans, prepuce, meatus, shaft, scrotum
- Female sites - labia, clitoris, periurethral area, perineum, vagina, cervix (flat lesions)
- Pruritus
- Irritation
- Bleeding (result of trauma)
- Perianal area (both sexes)
- Subclinical HPV infection
- May be detected by Pap test
Many patients notice painless or mildly symptomatic growths that can coalesce or remain discrete. Symptoms such as pruritus, irritation, or bleeding often prompt evaluation, but subclinical infection may be present even when visible warts are absent.
| Category | Examples from clinical description |
|---|---|
| Typical morphology | Soft, sessile lesions with smooth to very rough surface; multiple fingerlike projections |
| Perianal appearance | Condylomata are usually rough and cauliflower-like |
| Common male sites | Frenulum, corona, glans, prepuce, meatus, shaft, scrotum |
| Common female sites | Labia, clitoris, periurethral area, perineum, vagina, cervix (flat lesions) |
| Symptoms | Pruritus, irritation, bleeding after trauma |
| Subclinical infection | May be detected by Pap test in the absence of obvious warts |
What Causes Disease?
Human papillomaviruses. These are circular, double-stranded DNA molecules. There are over 70 HPV subtypes. The common cause of venereal warts is types 6 and 11. Cervical dysplasia and carcinoma in situ are likely caused by types 16, 18, 31, 33, and 35.
Risk Factors
- Young adult
- Sexually active
- Not using condoms
- Possibly subclinical infection
- Young age of commencing sexual activity
- Cigarette smoking
- Poor hygiene
- Pregnancy
- Caucasian
- History of genital warts
Risk increases with early onset of sexual activity, multiple partners, and other sexually transmitted infections. Smoking and immunosuppression may further impair local defences and favour persistence of HPV infection.
Diagnosis of Disease
Differential Diagnosis
- Condyloma lata (flat warts of syphilis)
- Lichen planus
- Normal sebaceous glands
- Seborrhoeic keratosis
- Molluscum contagiosum
- Keratomas
- Scabies
- Crohn disease
- Skin tags
- Melanocytic naevi
- Vulvar intraepithelial neoplasia
- Buschke-Lowenstein tumour
Because many benign and premalignant lesions can mimic condyloma acuminata, careful examination and, when indicated, biopsy are important for accurate diagnosis.
Laboratory
Serologic test for syphilis - negative
Drugs that may alter lab results: N/A
Disorders that may alter lab results: N/A
Pathological Findings
- Possible cervical dysplasia in females
- Benign
- Well organised basal layer
- Underlying infiltration of lymphocytes
- Plasma cells
- Hyperplastic epithelial changes
- Basement membrane intact
- Sometimes difficult to differentiate from squamous cell carcinoma
Special Tests
Aceto-whitening: Subclinical lesions can be visualised by wrapping the penis with gauze soaked with 5% acetic acid for 5 minutes. Using a ten X hand lens or colposcope, warts appear as tiny white papules. A shiny white appearance of the skin represents foci of epithelial hyperplasia (subclinical infection). Not highly specific, low positive predictive value.
Diagnostic Procedures
- Biopsy with highly specialised identification techniques (not clinically useful). HPV DNA detection is done by PCR on biopsy tissue.
- Colposcopy, antroscopy, anoscopy, Pap smear
- Urethroscopy may be required to visualise intraurethral lesions
Treatment (Medical Therapy)
Appropriate Health Care
Outpatient
General Measures
- May resolve on their own
- Treatment is determined by the location and size of warts
- Small warts may be treated with topical applications
- Cryotherapy
- Change therapy if no improvement after 3 treatments, no complete clearance after 6 treatments, or therapy exceeding manufacturer's recommendations
- Appropriate screening and counselling of partners
Management is individualised and often requires repeated visits. Counselling about the chronic, recurrent nature of HPV infection helps set realistic expectations.
Surgical Measures
- Larger warts require laser treatment or electrocoagulation
- Surgical excision for large warts
- Intraurethral, external (penile and perianal), anal, and oral lesions can be treated with fulgurating CO2 laser. Oral or external penile/perianal lesions can also be treated with electrocautery or surgery.
Activity
No restrictions
Diet
No special diet
Patient Education
- Explain preventive measures and the chronic nature of the infection
- Numerous pamphlets on HPV, STD prevention, condom use
- Emphasise the need for women to get regular Pap smears
Clear communication about transmission, condom use, vaccination, and the importance of follow-up care is essential for long-term management.
Medications (Drugs, Medicines)
Drug(s) of Choice
- Imiquimod (Aldara) 5% cream applied overnight 3 times weekly until warts clear for up to 16 weeks
- Cryotherapy - liquid nitrogen is applied to warts in 5-10 second bursts. Usually requires 2-3 weekly sessions.
- Podophyllin in tincture of Benzoin. Apply directly to warts. Leave on for 1-4 hours, then wash off. Repeat treatment every 7 days until gone (in office procedure) OR
- Podofilox (Condylox) - for external warts. Apply to external warts every 12 hours (allowing to dry) for 3 consecutive days. May repeat after 4 days (home application).
- Trichloroacetic acid - 25-85%. Apply only to warts. Use powder/talc to remove unreacted acid. Repeat in office at weekly intervals.
- Topical cidofovir gel - undergoing trials; applied once daily for 5 days every other week for maximum of 6 cycles
- Intralesional interferon has been shown to be effective in refractory cases and should be reserved for such cases
Choice of therapy depends on lesion size, number, location, patient preference, pregnancy status, cost, and provider experience. More than one treatment modality may be needed over time.
| Approach | Examples from regimen list | Typical setting or notes |
|---|---|---|
| Patient-applied topical therapy | Imiquimod cream; Podofilox (Condylox) for external warts | Used at home following instructions; requires adherence for weeks |
| Provider-applied destructive therapy | Cryotherapy with liquid nitrogen; trichloroacetic acid | Performed in the office; often repeated at weekly or periodic intervals |
| Provider-applied topical cytotoxic therapy | Podophyllin in tincture of Benzoin | Applied to limited areas; washed off after a few hours |
| Adjunctive or refractory-case therapy | Topical cidofovir gel (trials); intralesional interferon | Considered for resistant lesions; used under specialist guidance |
Contraindications:
- Podophyllin - do not use during pregnancy or on oral, cervical, urethral, or perianal warts. Can use on small number of vaginal warts with careful drying after application.
- Cryotherapy - cryoglobulinaemia
Precautions:
- Podophyllin - to minimise local and systemic reactions, wash treated areas 1-4 hours after application and use ointments to protect surrounding skin from contact with podophyllin
- Cryotherapy - none
- Electrocautery - don't use in patient with pacemaker
Significant possible interactions: N/A
Alternative Drugs
- External (penile and perianal)
- Podophyllin
- Podofilox (Condylox) self-treatment
- Intralesional interferon
- Small study of topical BCG use for penile lesions
- Urethral meatus
- Podophyllin
- Topical fluorouracil
- Anal
- Trichloroacetic acid (TCA) - apply weekly
- Topical fluorouracil
- Oral
- Trichloroacetic acid is ideal for isolated lesions in pregnant women
- Oral cimetidine 30-40 mg/kg divided tid for 3 months in children with genital and perigenital condyloma. Used as a primary and adjunctive therapy.
Patient Monitoring
- Every 2 weeks for treatment until clear
- Pap test every 1 year for indefinite period
- Biopsy for persistent warts
- Monitor sex partners
- Treatment does not decrease infectivity
Ongoing follow-up is essential because recurrences are common and infection can persist even after visible warts disappear.
Prevention / Avoidance
- Use of condoms by male sexual partners of individuals who have been treated for HPV infection
- Use of condoms by infected men (preventive effects not adequately evaluated; 40% of infected men have scrotal warts)
- Abstinence by women until treatment completed
- Circumcision may prevent recurrence in some men
- HPV vaccine - phase II trial in progress, appears encouraging
Possible Complications
- Cervical dysplasia
- Malignant change: Progression to cancer rarely, if ever, occurs
- Male urethral obstruction
- The prevalence of high grade dysplasia (HGD) and cancer in anal canal is higher in HIV-positive than in HIV-negative patients, probably because of HPV activity
Expected Course / Prognosis
- Warts clear with treatment or spontaneous regression
- Recurrences: Frequent and may necessitate repeated treatment
- Some studies identified 3 independent risk factors for condyloma relapse: Positive HIV, male sex, and Langerhans' cells - LCs/mm anal tissue (15 vs. 30)
- Without treatment: May remain stable, worsen, or resolve completely
- Asymptomatic infection persists indefinitely
Long-term prognosis depends on immune status, coexisting infections, and adherence to follow-up and screening recommendations, particularly for cervical and anal dysplasia.
Miscellaneous
Associated Conditions
- 90% of cervical cancer contains evidence of HPV infection
- Gonorrhoea
- Syphilis
- AIDS
- Chlamydia
- Other sexually transmitted disease
Age-Related Factors
Young adults, infants and children
Pediatric: Consider sexual abuse if seen in children;
although can acquire by other means (eg, transfer from wart on child's hand)
Geriatric: N/A
Others:
- Venereal warts are increasing in an ever younger population. A recent study of 487 college women showed an infection rate of 48%.
- Increased size and number in immunocompromised states
Pregnancy
- Warts often grow larger in pregnancy and regress spontaneously after delivery. Use cryotherapy.
- Virus does not cross the placenta. Treatment during pregnancy is somewhat controversial. C-section is not indicated.
- HPV can be transmitted to infant at time of delivery and cause laryngeal papillomas, a rare and life-threatening condition
Synonyms
- Genital warts
- Venereal warts
- Papilloma acuminatum
International Classification of Diseases
078.11 Condyloma acuminata

















