Management of Tinea Capitis
Definition of Tinea Capitis
The term tinea capitis refers to dermatophyte infections of the scalp and hair.
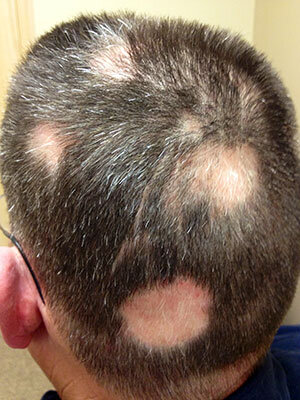
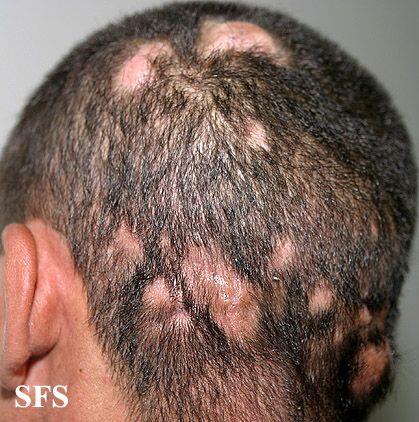
This infection most often affects children and typically presents with patchy hair loss, scaling, or broken hairs. Some patients may develop inflammation with pustules or boggy plaques, while others have only subtle flaking, which can delay recognition.
Geographic Distribution of Tinea Capitis
The condition occurs worldwide, but is most prevalent in Africa, Asia, and southern and eastern Europe, where it is the most common form of dermatophytosis. Improved standards of hygiene and prompt eradication of sporadic infection have led to a marked decline in the incidence of tinea capitis in North America and western Europe. Favus was previously distributed worldwide, but is now confined to North Africa, the Middle East, and parts of southern and eastern Europe.
Patterns of migration, urban crowding, and close contact among school-aged children also influence local epidemiology. As a result, clinicians in low-incidence countries may still encounter imported cases or clustered outbreaks.
Causal Organisms
Tinea capitis is caused by a number of Trichophyton and Microsporum species. M. canis is a frequent cause of the condition in western Europe, but T. violaceum is predominant in eastern and southern Europe and North Africa. T. tonsurans is predominant in North America, and is becoming more common in the UK.
Tinea capitis due to anthropophilic Microsporum species is a contagious disease endemic in many countries. It is primarily a disease of children, is more common in males than females, and is most prevalent between 6 and 10 years of age. The disease seldom persists beyond the age of 16. Large outbreaks often occur in schools or other places where children congregate. Zoophilic Microsporum and Trichophyton species are seldom responsible for more than minor outbreaks of human infection. Household pets, such as dogs and cats, are a common source of infection, and feral cats are another prolific source of M. canis.
Tinea capitis due to anthropophilic Trichophyton species is also a contagious disease. It is most common in boys under the age of 12.
T. schoenleinii is considered the sole aetiologic agent of favus, although infections with other dermatophytes, such as M. gypseum, T. verrucosum and T. violaceum, can sometimes produce somewhat similar lesions. Although T. schoenleinii is an anthropophilic dermatophyte, favus is less contagious than other forms of tinea capitis due to Microsporum or other Trichophyton species. It is usually contracted in childhood and may persist into adult life. Debilitated or malnourished children, or children with a chronic disease such as tuberculosis, are more susceptible to this infection. Instances have been reported in which several generations of the same family were affected.
Together, these organisms account for most cases worldwide. Regional differences reflect local reservoirs (human, animal, or environmental) and patterns of crowding and hygiene.
| Region or context | Organisms mentioned | Typical characteristics |
|---|---|---|
| Western Europe | M. canis | Frequent cause of tinea capitis; often linked to household pets or feral cats. |
| Eastern and southern Europe, North Africa | T. violaceum | Predominant anthropophilic species; supports person-to-person spread among children. |
| North America | T. tonsurans | Predominant organism; contagious, with cases clustered in schools and families. |
| United Kingdom | T. tonsurans (emerging) | Becoming more common, reflecting changing epidemiology and travel patterns. |
| Favus-endemic areas (North Africa, Middle East, parts of southern and eastern Europe) | T. schoenleinii | Sole aetiologic agent of favus; anthropophilic dermatophyte, less contagious but may persist into adult life. |
| Animal-associated infections | Zoophilic Microsporum and Trichophyton species, especially M. canis | Often related to contact with dogs, cats, or farm animals; usually cause minor human outbreaks. |
| Host factors | - | Children 6-10 years old; male predominance; increased risk with malnutrition, chronic disease, or close-contact settings such as schools. |
Management of Tinea Capitis
If possible, specimens for mycological examination should be taken before starting treatment. If oral treatment is being considered, mycological confirmation of the clinical diagnosis is essential before treatment is commenced.
Terbinafine (250 mg/day for 2 weeks) and itraconazole (100 mg/day for 2 weeks) have both proved effective in the oral treatment of tinea capitis, but neither compound is licensed for this indication at present. The duration of griseofulvin treatment depends on the nature of the infection and the clinical response; some infections can take up to 3 months to clear. The usual dosage is 10 mg/kg and this should be given after food. Mycological tests should be repeated 1 month after starting treatment and again before discontinuing the drug.
Various topical imidazole preparations can be used to treat localised scalp lesions, including clotrimazole, miconazole and sulconazole. These medicines are safe and side effects after local application are uncommon.
Systemic therapy is the cornerstone of treatment for most cases of tinea capitis, with topical agents used as adjuncts to reduce surface fungal load and limit transmission. Close follow-up with repeat mycological testing helps confirm cure and guide the duration of therapy.
| Therapy | Role in management | Examples and dosing from text | Duration from text |
|---|---|---|---|
| Systemic terbinafine | Oral treatment option for tinea capitis* | Terbinafine 250 mg/day | 2 weeks |
| Systemic itraconazole | Alternative oral treatment option* | Itraconazole 100 mg/day | 2 weeks |
| Systemic griseofulvin | Established oral therapy; duration depends on clinical response | Griseofulvin 10 mg/kg/day, given after food | Up to 3 months in some infections |
| Topical imidazoles | Adjunct therapy for localised scalp lesions | Clotrimazole, miconazole, sulconazole | Used during systemic treatment and until lesions improve |
| Diagnostic mycology | Guides initiation and completion of systemic therapy | Mycological tests at baseline, 1 month after starting treatment, and before discontinuation | As specified in the text |
* The text notes that terbinafine and itraconazole have proved effective but are not licensed for this indication at present.
To prevent epidemics of anthropophilic tinea capitis due to M. audouinii from developing, all contacts of infected children should be examined with Wood's light. Contacts of children with T. tonsurans infection can be screened using the hair brush sampling method. It is seldom practical to exclude infected children from school, in view of the long duration of treatment.
Screening close contacts, examining pets when appropriate, and educating families about not sharing combs, hats, or hair accessories can help limit spread while treatment is underway.

















