Isoniazid
Dosages
Isoniazid 300 mg
| Quantity | Price per tablet | Total price | |
|---|---|---|---|
| 90 | A$0.65 | A$58.58 | |
| 120 | A$0.60 | A$71.60 | |
| 180 | A$0.54 | A$97.64 | |
| 270 | A$0.51 | A$137.99 | |
| 360 | A$0.49 | A$177.04 |
Payment & Delivery
Your order is carefully packed and ships within 24 hours. Here is what a typical package looks like.
Sized like a regular personal letter (approximately 24x11x0.7 cm), with no indication of what is inside.



| Delivery Method | Estimated delivery |
|---|---|
| Express Free for orders over A$390.54 | Estimated delivery to Australia: 4-7 days |
| Standard Free for orders over A$260.36 | Estimated delivery to Australia: 14-21 days |










Discount Coupons
- Australia Day - 26 January 2026 10% AUSDAY10
- ANZAC Day - 25 April 2026 8% ANZAC8
- Boxing Day - 26 December 2026 12% BOXING12
Brand Names
| Country | Brand Names |
|---|---|
 Argentina Argentina | Isoniac |
 Austria Austria | INH Agepha |
 Belgium Belgium | Nicotibine Rimifon |
 Bulgaria Bulgaria | Isonid Rimicid |
 Canada Canada | Isotamine |
 Czechia Czechia | Nidrazid |
 Egypt Egypt | Isocid forte |
 Finland Finland | Tubilysin |
 France France | Rimifon |
 Germany Germany | Dipasic Gluronazid Isozid Isozid comp N Tb-Phlogin cum B6 tebesium tebesium-s |
 Greece Greece | Dianicotyl Isozid Nicozid |
 Hong Kong Hong Kong | Trisofort |
 Hungary Hungary | Isonicid |
 Iceland Iceland | Tibinide |
 India India | Isokin Isonex Rifacom E-Z |
 Israel Israel | Inazid |
 Italy Italy | Cin Nicazide Nicizina Nicozid |
 Japan Japan | Hydra Hydrazide |
 Mexico Mexico | Dipasic Erbazid Hidrasix Pas Hain Valifol |
 Pakistan Pakistan | Aceta Amsozide Isonex Forte |
 Philippines Philippines | Isonid |
 Portugal Portugal | Hidrazida |
 Romania Romania | Bitub |
 Slovenia Slovenia | INH Agepha |
 Spain Spain | Anidrasona Cemidon Cemidon B6 Dipasic Hidrastol Pyreazid Rimifon |
 Sweden Sweden | Tibinide |
 Switzerland Switzerland | Rimifon |
 Taiwan Taiwan | Duracrin I.N.A.H. Iscotin |
 Turkey Turkey | I.N.H. |
 United Kingdom United Kingdom | Inapsade Rimifon |
 United States United States | Laniazid Nydrazid |
Description
Isoniazid is a first-line anti-tuberculosis medicine used to treat active tuberculosis (together with other medicines) and to help prevent active disease in people with latent tuberculosis (TB) infection. In Australia, it should only be used as prescribed, with appropriate dosing and monitoring, especially for liver safety, and in line with your clinician's instructions.

Uses
Active tuberculosis
Isoniazid is used with other anti-tuberculosis medicines to treat clinical tuberculosis.
In Australia, national tuberculosis guidance recommends several multi-drug regimens for the treatment of culture-positive pulmonary tuberculosis. These regimens have a minimum duration of 6 months (26 weeks) and include an initial intensive phase (2 months) followed by a continuation phase (usually either 4 or 7 months). Isoniazid is considered a first-line anti-tuberculosis medicine for the treatment of all forms of tuberculosis caused by Mycobacterium tuberculosis known or presumed to be susceptible to the drug.
In Australia, isoniazid may be available as a single-ingredient product or in fixed-dose combination products used for tuberculosis treatment, depending on local registration and supply. While oral isoniazid is preferred for treating tuberculosis, the medicine may also be given IM for initial treatment or retreatment when it cannot be taken by mouth.
Latent tuberculosis infection
Isoniazid is usually used on its own to treat latent tuberculosis infection and help prevent clinical tuberculosis from developing. In the past, terms such as "preventive therapy" or "chemoprophylaxis" were used to describe a simple medicine regimen (for example, isoniazid monotherapy) used to prevent active tuberculosis disease in people known or likely to be infected with M. tuberculosis. However, because this type of regimen rarely results in true primary prevention (that is, preventing infection in people exposed to infectious tuberculosis), the American Thoracic Society (ATS) and Centers for Disease Control and Prevention (CDC) now state that "treatment of latent tuberculosis infection" is a more accurate term than "preventive therapy" and may help improve understanding and wider use of this tuberculosis control strategy.
People at risk of developing tuberculosis include those who have recently been infected with M. tuberculosis and those with clinical conditions that increase the risk of latent tuberculosis infection progressing to active disease. The chance that a positive tuberculin test reflects true infection with M. tuberculosis is influenced by how common infection is in the population being tested. The ATS and Centers for Disease Control and Prevention (CDC) state that, because the general population of the US has an estimated M. tuberculosis infection rate of 5-10% and the annual incidence of new tuberculosis infection without known exposure is estimated at 0.01-0.1%, the tuberculin skin test has a low positive predictive value in people without known or likely exposure to M. tuberculosis. To focus resources on identifying those at risk of developing tuberculosis and reduce false-positive tuberculin test results, the ATS and Centers for Disease Control and Prevention (CDC) currently recommend targeting tuberculin testing to high-risk groups and discouraging it in low-risk groups. The ATS and Centers for Disease Control and Prevention (CDC) currently define positive tuberculin reactions in terms of 3 cut-off points (levels of induration), based on the sensitivity, specificity and prevalence of tuberculosis in different groups: 5 mm or more of induration for people at highest risk of developing clinical tuberculosis, 10 mm or more for those with a higher probability of infection or with clinical conditions that increase progression to active tuberculosis, and 15 mm or more for people at low risk, in whom tuberculin testing is generally not indicated.
Key groups for tuberculin testing and treatment
- Individuals with HIV infection
- Those with an induration reaction of 5 mm or greater should receive LTBI therapy unless it is contraindicated.
- Preventive therapy is recommended even if the tuberculin test is negative when there is known exposure to active tuberculosis.
- Isoniazid therapy may be beneficial for tuberculin-negative children born to mothers with HIV infection.
- Close contacts of people with tuberculosis
- Contacts with a significant reaction (≥5 mm) should be treated for LTBI, regardless of age.
- Children under 5 years should be treated regardless of test results because they are more vulnerable to disease.
- Immunocompromised individuals
- Those receiving prolonged corticosteroid therapy or organ transplants should be treated if they have a significant tuberculin reaction.
- Immunosuppressed people who are contacts of active tuberculosis cases should also receive treatment.
- Individuals with a prior tuberculosis history
- Those with healed but untreated tuberculosis should receive LTBI therapy, regardless of age.
- High-risk population groups
- Recent immigrants from high-prevalence countries, residents of long-term care facilities, and healthcare workers exposed to tuberculosis patients should be considered for treatment if they have significant tuberculin reactions.
- Children and adolescents
- Infants and children exposed to high-risk adults should be treated if they have a significant tuberculin reaction.
Testing and treatment considerations
- Routine testing is not recommended for low-risk populations, but treatment may be considered for those with significant reactions.
- Before starting isoniazid therapy, patients must be checked for active tuberculosis and liver problems to make sure there are no contraindications.
This streamlined approach helps ensure that vulnerable groups receive appropriate screening and treatment to prevent latent tuberculosis from progressing to active disease.
Isoniazid monotherapy
Isoniazid monotherapy is recommended for treating latent tuberculosis infection (LTBI) in both adults with HIV infection and those without it, with a preferred regimen of 9 months taken daily or twice weekly. For infants and children, a similar 9-month regimen is recommended, although some experts suggest extending treatment to 12 months for children with HIV infection. While the 9-month regimen is preferred, a 6-month regimen can be used for adults without HIV infection, offering substantial protection and potentially lower costs. However, it is not recommended for children or for those with evidence of prior tuberculosis. Research suggests that regimens shorter than 6 months are ineffective, and a large study confirmed that a 6-month course is more effective than shorter options. The ATS and Centers for Disease Control and Prevention (CDC) emphasise the importance of sticking to treatment, recommending at least 270 doses for the 9-month regimen and 180 doses for the 6-month option. Intermittent dosing should be directly observed to help ensure adherence. If treatment is interrupted for more than two months, a medical review is needed before therapy is restarted.
Alternative regimens
While isoniazid monotherapy is generally the regimen of choice for treating latent tuberculosis infection, a 4-month regimen of daily rifampin monotherapy can be used as an alternative in both HIV-positive and HIV-negative patients, especially when isoniazid cannot be used because of resistance or intolerance.
Limited data suggest that a short-course (for example, 2-month) regimen of rifampin and pyrazinamide given daily is effective in treating latent tuberculosis infection in patients with HIV infection, and the ATS and Centers for Disease Control and Prevention (CDC) state that the effectiveness of this regimen is not expected to differ in HIV-negative patients. However, liver toxicity, including some fatal cases, has been reported in patients receiving rifampin and pyrazinamide regimens for latent tuberculosis. Although multi-drug regimens containing rifampin and pyrazinamide are still recommended for active tuberculosis, the ATS, Centers for Disease Control and Prevention (CDC), and IDSA now state that regimens containing both rifampin and pyrazinamide generally should not be offered for latent tuberculosis in either HIV-infected or HIV-negative individuals.
HIV-infected individuals
Factors to consider when choosing the right regimen for latent tuberculosis infection in people with HIV infection include whether the infecting organism is likely to be susceptible to isoniazid (isoniazid is the preferred medicine for isoniazid-susceptible M. tuberculosis), the potential for interactions between rifampin and HIV protease inhibitors or non-nucleoside reverse transcriptase inhibitors (NNRTIs), and the possibility of severe liver injury with pyrazinamide-containing regimens. If the infecting organism is resistant to isoniazid and rifampin, treatment choice requires consultation with public health authorities.
Recommendations for treating latent tuberculosis infection in adults with HIV infection are generally similar to those for HIV-negative adults. However, the 6-month isoniazid monotherapy regimen is usually not recommended, and rifabutin monotherapy may be needed instead of rifampin monotherapy if there are concerns about interactions with antiretroviral medicines the patient may be taking. The ATS and Centers for Disease Control and Prevention (CDC) recommend that adults and adolescents with HIV infection and latent M. tuberculosis infection receive a 9-month regimen of isoniazid given daily or twice weekly; a 4-month regimen of rifampin or rifabutin given daily; or a 2- to 3-month regimen of rifampin and pyrazinamide given daily (this regimen is no longer recommended for most patients).
For infants and children with HIV infection, recommended regimens for latent tuberculosis infection are a 9- to 12-month regimen of isoniazid given daily or twice weekly, or a 4- to 6-month regimen of rifampin given daily.
Pregnant women
For pregnant women who are at risk of latent tuberculosis infection progressing to active disease, particularly those with HIV infection or recent infection, the ATS and Centers for Disease Control and Prevention (CDC) state that starting or stopping therapy for latent tuberculosis infection should not be delayed because of pregnancy alone, even during the first trimester. For women at lower risk of active disease, some experts recommend delaying treatment until after delivery. Patients with HIV infection or radiographic evidence of prior tuberculosis should receive 9 rather than 6 months of isoniazid therapy. The ATS and Centers for Disease Control and Prevention (CDC) state that some experts would use rifampin and pyrazinamide as an alternative regimen for latent tuberculosis infection in pregnant women with HIV infection, although pyrazinamide should be avoided during the first trimester. The ATS and Centers for Disease Control and Prevention (CDC) state that a regimen of isoniazid given daily or twice weekly for 9 or 6 months is recommended in these pregnant women who do not have HIV infection.
Drug-resistant latent tuberculosis infection
In people likely to be infected with M. tuberculosis organisms that are resistant to both isoniazid and rifampin and who are at high risk of developing tuberculosis, the ATS and Centers for Disease Control and Prevention (CDC) recommend regimens containing pyrazinamide and ethambutol or pyrazinamide and a quinolone anti-infective (for example, levofloxacin or ofloxacin) for 6-12 months if the organisms from the index case are known to be susceptible to these medicines. Immunocompetent contacts may be managed with observation alone or treated with such regimens for 6 months; immunosuppressed individuals, including those with HIV infection, should be treated for 12 months. Clinicians should review the drug-susceptibility pattern of the M. tuberculosis strain isolated from the source patient before selecting a regimen for potentially multidrug-resistant tuberculosis infection. In people likely to have been infected with M. tuberculosis organisms resistant to both isoniazid and rifampin, the choice of medicines for latent infection requires expert consultation. Before starting therapy for latent tuberculosis infection in patients with suspected multidrug-resistant tuberculosis, a careful assessment is needed to rule out active disease.
In Australian practice, until susceptibility test results are available, child contacts who are likely to have been infected by an index case with isoniazid-resistant tuberculosis may receive both rifampin and isoniazid. If the index case is confirmed to be excreting organisms that are completely resistant to isoniazid, isoniazid should be stopped and rifampin should be given for at least six months. Expert advice is recommended when making decisions about therapy for latent tuberculosis infection in children with isoniazid- and/or rifampin-resistant M. tuberculosis.
Dosage
Oral and IM doses of isoniazid are identical.
Active tuberculosis
In the treatment of clinical tuberculosis, isoniazid should not be given alone. The medicine is considered a first-line agent for treating all forms of tuberculosis. Treatment should continue for long enough to prevent relapse. In Australia, the minimum recommended treatment duration for patients with culture-positive pulmonary tuberculosis is 6 months (26 weeks), with an initial intensive phase (2 months) followed by a continuation phase (usually either 4 or 7 months). Completion of treatment is assessed more accurately by the total number of doses taken rather than by duration alone.
Adult dosage
The ATS, Centers for Disease Control and Prevention (CDC), and IDSA recommend that adults and children 15 years of age or older receive an isoniazid dose of 5 mg/kg (up to 300 mg) once daily when isoniazid is used with other anti-tuberculosis medicines.
When an intermittent multi-drug regimen is used to treat tuberculosis, the ATS, Centers for Disease Control and Prevention (CDC), and IDSA recommend that adults and children 15 years of age or older receive isoniazid at a dose of 15 mg/kg (up to 900 mg) once, twice, or three times weekly.
Paediatric dosage
Infants and children may tolerate larger doses of isoniazid than adults and may receive up to 10-20 mg/kg once daily, depending on the severity of the disease. In Australian clinical practice, when isoniazid is used in daily multi-drug regimens in paediatric patients, a dose of 10-15 mg/kg (up to 300 mg) daily is commonly used. Caution is advised because using more than 10 mg/kg daily together with rifampin may increase the risk of liver toxicity.
When an intermittent multi-drug regimen is used for the treatment of tuberculosis in paediatric patients, the ATS, Centers for Disease Control and Prevention (CDC), IDSA, and AAP recommend an isoniazid dose of 20-30 mg/kg (up to 900 mg) twice weekly.
Fixed-combination preparations
When isoniazid is given as the fixed combination containing isoniazid and rifampin (Rifamate®) as part of a multi-drug regimen for pulmonary tuberculosis, the usual adult dose of Rifamate® is 2 capsules (600 mg of rifampin and 300 mg of isoniazid) once daily.
Although the fixed-combination preparation was developed for daily regimens, the ATS, Centers for Disease Control and Prevention (CDC), and IDSA state that Rifamate® can be used in twice-weekly regimens as long as additional isoniazid is given at the same time.
When used in an intermittent multi-drug regimen, these experts state that two capsules of Rifamate® (600 mg of rifampin and 300 mg of isoniazid) and an additional 600 mg of isoniazid (900 mg of isoniazid total) may be given twice weekly using directly observed therapy (DOT).
The manufacturer states that Rifamate® should not be used for the initial treatment of tuberculosis, but only after the effectiveness of the rifampin and isoniazid doses contained in the fixed-combination preparation has been established by titrating the individual components in the patient.
When isoniazid is given as the fixed combination containing isoniazid, rifampin, and pyrazinamide (Rifater®) in the initial phase (for example, the initial 2 months) of multi-drug therapy for pulmonary tuberculosis, the manufacturer states that the adult dose of Rifater® given as a single daily dose is 4 tablets (480 mg of rifampin, 200 mg of isoniazid, 1.2 g of pyrazinamide) in patients weighing 44 kg or less, 5 tablets (600 mg of rifampin, 250 mg of isoniazid, and 1.5 g of pyrazinamide) in those weighing 45-54 kg, and 6 tablets (720 mg of rifampin, 300 mg of isoniazid, 1.8 g of pyrazinamide) in patients weighing 55 kg or more. In individuals weighing more than 90 kg, additional pyrazinamide may need to be given with the fixed-combination preparation to achieve an adequate dose of this medicine.
The ratio of rifampin, isoniazid, and pyrazinamide in Rifater® may not be appropriate in children or adolescents under 15 years of age because children are usually given higher mg/kg doses of isoniazid than adults.
Latent tuberculosis infection
Isoniazid is usually the only anti-tuberculosis medicine used for at least six months to treat latent tuberculosis infection. Every effort should be made to ensure adherence for at least six months, since preventive therapy of shorter duration appears to provide little benefit. If medicine administration cannot be directly observed, spot testing of urine for isoniazid metabolites has been recommended to assess adherence.
The ATS and Centers for Disease Control and Prevention (CDC) currently recommend a 9-month daily isoniazid regimen or, alternatively, a 9-month twice-weekly isoniazid regimen for adults regardless of HIV infection status. Continuing isoniazid therapy for latent tuberculosis infection for longer than 12 months provides no additional benefit. It is also recommended that isoniazid therapy for latent tuberculosis infection be continued for 9-12 months in infants and children with HIV infection.
The ATS and Centers for Disease Control and Prevention (CDC) state that completion of therapy for latent tuberculosis infection is determined more accurately by the total number of doses and should not be based only on treatment duration. The 9-month daily isoniazid regimen should consist of at least 270 doses given within 12 months (allowing for interruptions in the usual 9-month regimen), and the 6-month daily isoniazid regimen should consist of at least 180 doses given within 9 months. Isoniazid regimens in which the medicine is given twice weekly should consist of at least 76 doses administered within 12 months (for the 9-month regimen) or at least 52 doses within 9 months (for the 6-month regimen).
Administration
Isoniazid is usually taken by mouth. The medicine may be given by IM injection when oral therapy is not possible. The fixed-combination preparation containing isoniazid and rifampin (Rifamate®) and the fixed-combination preparation containing isoniazid, rifampin, and pyrazinamide (Rifater®) should be taken either 1 hour before or 2 hours after a meal; the manufacturer states that Rifater® should be taken with a full glass of water.
Solutions of isoniazid should be sterilised by autoclaving.
Important safety information
Liver function tests should be carried out periodically in patients taking isoniazid. Patients should also be asked every month about signs and symptoms of liver disease and told to report any early symptoms of hepatitis to their doctor, such as persistent tiredness, weakness, or fever lasting more than 3 days; feeling unwell; nausea; vomiting; or unexplained loss of appetite. If these symptoms appear, or if there are signs suggesting liver damage, isoniazid should be stopped promptly, as continued use has been reported to cause more severe liver injury in these patients.
Some clinicians recommend stopping isoniazid if serum aminotransferase concentrations are more than 3-5 times the upper limit of normal, or if the patient develops signs of hepatitis. Patients who have had signs or symptoms of liver damage during isoniazid treatment should generally be given alternative antituberculosis medicines. If isoniazid must be started again, it should only be restarted after liver-related symptoms and laboratory abnormalities have resolved. Isoniazid should be reintroduced in very small, gradually increasing doses and stopped immediately if there is any sign of the liver being affected again.
The AAP states that hepatitis during isoniazid therapy is rare in children and that routine measurement of serum aminotransferase concentrations is not recommended. However, liver function tests should be monitored about monthly during the first several months of treatment in children with severe tuberculosis, especially meningitis and disseminated disease.
The AAP also states that liver function tests should be monitored in patients with current or recent liver disease, those receiving a high daily dose of isoniazid (more than 10 mg/kg/day) together with rifampin and/or pyrazinamide, those who are pregnant or within 6 weeks after giving birth, those with clinical evidence of hepatotoxicity, those with hepatobiliary disease from other causes, and those taking other hepatotoxic drugs at the same time, especially anticonvulsants. In most other patients, monthly clinical review for 3 months, followed by review every 1-3 months to watch for signs of hepatitis or other side effects, is appropriate.
Isoniazid should be used with caution in people who drink alcohol daily, people who inject illicit drugs, patients with chronic liver disease or severe renal impairment, and those with a history of previous treatment in which isoniazid was stopped because of side effects such as headache, dizziness, or nausea that may possibly, but not definitely, have been related to the drug. Minor dose adjustments may be needed in patients with severe renal impairment. Limited data from a retrospective analysis of deaths linked to isoniazid-associated hepatitis suggest that the risk of fatal hepatitis may be higher in women, particularly Black and Hispanic women, and during the postpartum period.
Periodic eye examinations should be performed in patients who develop visual symptoms while taking the drug. The manufacturers recommend eye examinations, including ophthalmoscopy, before starting isoniazid and periodically during treatment even if visual symptoms do not occur; however, some clinicians question whether this precaution is necessary.
Isoniazid should be used with caution in patients who are malnourished or prone to neuropathy, such as people with diabetes or alcohol use disorder, and pyridoxine should generally be given at the same time. In Australian practice, pyridoxine is generally recommended as well in children and adolescents with very low milk and meat intake, in those with nutritional deficiencies, including all symptomatic children with HIV, in breastfed infants and their mothers, and in pregnant women.
Isoniazid is contraindicated in patients with acute liver disease or a history of previous isoniazid-associated liver injury. Although preventive therapy should be deferred in these patients, the ATS and CDC state that seropositivity for hepatitis B surface antigen is not a contraindication to this therapy. Isoniazid is also contraindicated in patients with a history of severe adverse reactions to the drug, including severe hypersensitivity reactions or drug fever, chills, and arthritis.
Side effects
Isoniazid is generally well tolerated at currently recommended doses. However, people who are slow acetylators of isoniazid and those with advanced HIV disease appear to have a higher rate of some side effects. Patients with poor nutrition are also at risk of peripheral neuritis, one of the most common side effects of isoniazid. Other neurological side effects include psychotic reactions and convulsions. Pyridoxine may be given to prevent or treat these effects. Optic neuritis has also been reported. Temporary increases in liver enzymes occur in 10 to 20% of patients during the first few months of treatment and usually return to normal despite continued treatment. Symptomatic hepatitis occurs in about 0.1 to 0.15% of patients given isoniazid alone, but this can increase with age, regular alcohol use, and chronic liver disease. The effect of acetylator status is uncertain.
Raised liver enzymes together with clinical signs of hepatitis, such as nausea, vomiting, or fatigue, may indicate liver damage. In these circumstances, isoniazid should be stopped while the patient is assessed and should only be reintroduced cautiously once liver function has recovered. Fatalities due to liver necrosis have occurred.
Interactions
The risk of hepatotoxicity may be increased in patients taking isoniazid with a rifamycin or other potentially hepatotoxic drugs, including alcohol. Isoniazid can inhibit the liver metabolism of a number of drugs, sometimes leading to increased toxicity. These include the antiepileptics carbamazepine, ethosuximide, primidone, and phenytoin; the benzodiazepines diazepam and triazolam; chlorzoxazone; theophylline; and disulfiram. Isoniazid has also been associated with increased concentrations and enhanced effects or toxicity of clofazimine, cycloserine, and warfarin.
Mechanism of action
Isoniazid may be bacteriostatic or bactericidal, depending on the concentration of the drug reached at the site of infection and the susceptibility of the infecting organism.
Although the exact mechanism of action of isoniazid has not been fully established, several mechanisms have been proposed, including interference with the metabolism of bacterial proteins, nucleic acids, carbohydrates, and lipids.
One of the drug's main actions appears to be inhibition of mycolic acid synthesis in susceptible bacteria, resulting in loss of acid-fastness and disruption of the bacterial cell wall. Isoniazid is active against susceptible bacteria only while they are undergoing cell division. Susceptible bacteria may undergo 1 or 2 divisions before multiplication is halted. Isoniazid is a highly specific agent and is active only against organisms of the genus Mycobacterium. Isoniazid is active in vitro and in vivo against M. tuberculosis, M. bovis, and some strains of M. kansasii.
Resistance
Natural and acquired resistance to isoniazid has been demonstrated in vitro and in vivo in strains of M. tuberculosis. In vitro, resistance to isoniazid develops stepwise. The mechanism of resistance may be related to the drug's failure to penetrate, or to be taken up by, resistant bacteria.
Resistant strains of bacteria that are initially susceptible develop rapidly if isoniazid is used alone to treat clinical tuberculosis. However, the development of resistance does not appear to be a major problem when the drug is used alone for preventive therapy. When isoniazid is combined with other antituberculosis agents in the treatment of clinical tuberculosis, the emergence of resistant strains may be delayed or prevented.
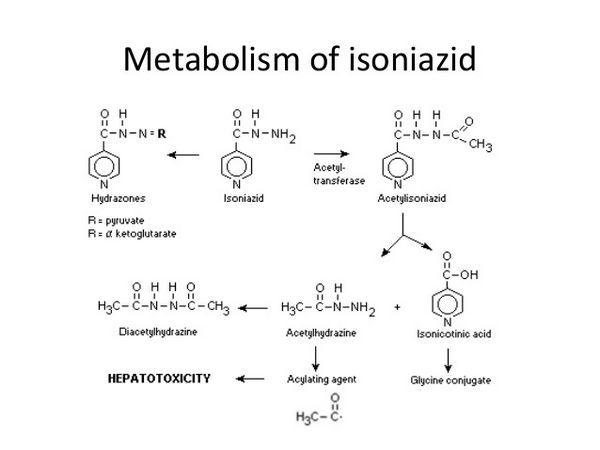
Pharmacokinetics
Isoniazid is readily absorbed from the gastrointestinal tract and after intramuscular injection. Peak concentrations of about 3 to 7 micrograms/mL appear in the blood 1 to 2 hours after an oral fasting dose of 300 mg. Food reduces the rate and extent of isoniazid absorption. Isoniazid is not considered to bind appreciably to plasma proteins and is distributed into all body tissues and fluids, including cerebrospinal fluid (CSF). It appears in fetal blood if given during pregnancy and is distributed into breast milk. The plasma half-life of isoniazid ranges from about 1 to 6 hours, with shorter half-lives in fast acetylators. The main metabolic pathway is acetylation of isoniazid to acetyl isoniazid by N-acetyltransferase in the liver and small intestine. In patients with normal renal function, more than 75% of a dose appears in the urine within 24 hours, mainly as metabolites. Small amounts of the drug are also excreted in the faeces. Isoniazid is removed by haemodialysis.
Distribution
Therapeutic concentrations of isoniazid have been detected in CSF and synovial fluid several hours after an oral dose. Diffusion into saliva is good, and it has been suggested that saliva concentrations could be used instead of serum concentrations in pharmacokinetic studies.
HIV-infected patients
Malabsorption of isoniazid and other antituberculous drugs may occur in patients with HIV infection and tuberculosis and may contribute to acquired drug resistance and reduced effectiveness of tuberculosis treatment.
Pregnancy
Isoniazid crosses the placenta, and average fetal concentrations of 61.5 and 72.8% of maternal serum or plasma concentration have been reported. The half-life of isoniazid may be prolonged in neonates.
Storage
Isoniazid preparations should be protected from light, air, and excessive heat. Isoniazid tablets should be stored in well-closed, light-resistant containers at a temperature below 40°C, preferably between 15-30°C. Tablets containing the fixed combination of rifampin, isoniazid, and pyrazinamide (Rifater®) should be protected from excessive humidity and stored at 15-30°C. Isoniazid injection should be protected from light and stored at a temperature below 40°C, preferably between 15-30°C; freezing should be avoided. At low temperatures, isoniazid in solution tends to crystallise, and the injection should be warmed to room temperature to redissolve the crystals before use.
Overdosage
Overdosage of isoniazid has caused nausea, vomiting, dizziness, slurred speech, blurred vision, and visual hallucinations, including bright colours and strange patterns. Symptoms of overdosage usually occur within 30 minutes to 3 hours after the drug is taken. After marked overdosage, respiratory distress and central nervous system depression, progressing rapidly from stupor to coma, severe intractable seizures, metabolic acidosis, acetonuria, and hyperglycaemia have occurred. If untreated or inadequately treated, isoniazid overdosage may be fatal.
Treatment of overdose
In the management of isoniazid overdosage, the airway should be secured and adequate breathing established immediately. Seizures may be controlled with IV diazepam or short-acting barbiturates and a dose of pyridoxine hydrochloride equal to the amount of isoniazid ingested. Generally, 1-4 g of pyridoxine hydrochloride is given IV, followed by 1 g IM every 30 minutes until the entire dose has been given. If seizures are controlled and the overdosage is recent, within 2-3 hours, the stomach should be emptied by gastric lavage.
Blood gases, serum electrolytes, glucose, and BUN should be measured. Blood should be typed and cross-matched in case haemodialysis is required. IV sodium bicarbonate should be given to control metabolic acidosis and repeated as needed; the dose should be adjusted according to laboratory test results.